0%
Agreement
Addressing Radiology Recommendations Collaboratively
In collaboration with the Department of Quality and Safety at BWH, the Department of Radiology launched a new initiative in October 2019 called Addressing Radiology Recommendations Collaboratively (ARRC).
The primary goals of this initiative are to:
Here's how ARRC works:
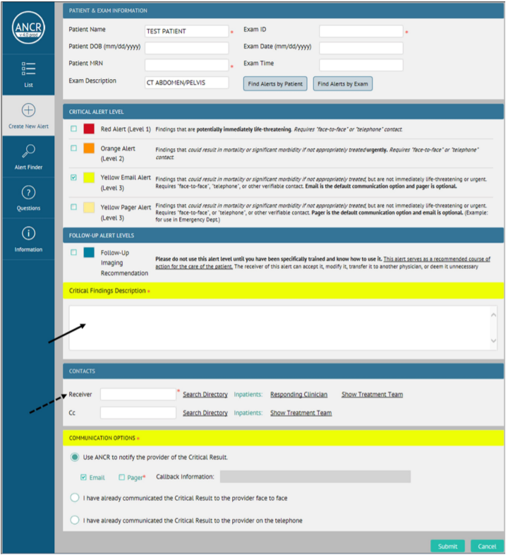
As part of ARRC, radiologists are asked to use a Blue ANCR to document an imaging follow-up recommendation.